What medications interact with local anesthesia?

Daniel Johnson
Published Feb 27, 2026
What medications interact with local anesthesia?
Most frequently checked interactions
- Advair Diskus (fluticasone / salmeterol)
- Ancef (cefazolin)
- Ativan (lorazepam)
- Benadryl (diphenhydramine)
- Cardizem (diltiazem)
- Crestor (rosuvastatin)
- Demerol (meperidine)
- Elavil (amitriptyline)
Does anesthesia affect antidepressants?
It is generally accepted that it is safe to administer anesthetics to patients on antidepressants; however, the anesthesia provider must be aware of the risk of potential drug–drug interactions; serotonin syndrome; hemodynamic changes; and/or bleeding issues.
What can you not take with tricyclic antidepressants?
Tricyclic antidepressants can cause harmful side effects if you take them with certain medications, including epinephrine (Epi-Pen) and cimetidine (Tagamet). Tricyclic antidepressants can increase the effects of epinephrine on your heart. This can lead to high blood pressure and problems with your heart rhythm.
What is the most concerning issue with tricyclic antidepressants?
Some tricyclic antidepressants are more likely to cause side effects that affect safety, such as: Disorientation or confusion, particularly in older people when the dosage is too high. Increased or irregular heart rate. More-frequent seizures in people who have seizures.
What are the risks related to the local Anaesthetic agent administered by injection?
Common local complications associated with local anesthesia are reported as pain at injection, needle fracture, prolongation of anesthesia and various sensory disorders, lack of effect, trismus, infection, edema, hematoma, gingival lesions, soft tissue injury, and ophthalmologic complications [2, 3].
Can you take paracetamol after local anesthetic?
When the local anaesthetic wears off, you may need some pain relief. If you’ve been prescribed pain relief, use it. Otherwise, you can take paracetamol (Panadol). Follow the instructions on the packet and take the tablets with food.
Can I have surgery while on antidepressants?
Some Antidepressants Linked to Surgical Risks. MONDAY, April 29 (HealthDay News) — Taking popular antidepressant drugs around the time of surgery may increase risks associated with the procedure, including bleeding, the need for a blood transfusion, hospital readmission and even death, a large new study suggests.
Should SSRIs be stopped before surgery?
So while the evidence doesn’t rule out an increase in bleeding risk, stopping antidepressants before surgery—especially the widely used selective serotonin reuptake inhibitors (SSRIs)—might worsen depression symptoms or lead to a potentially disastrous “discontinuation syndrome.” The authors conclude, “Therefore.
What are the precautions and contraindications for the tricyclic antidepressants?
Ask your doctor before taking TCAs if you:
- Are under age 25 or over age 65.
- Have diabetes, heart problems, or a thyroid disorder.
- Have any conditions affecting your urinary tract or an enlarged prostate.
- Have glaucoma.
- Have a liver disease.
- Have a history of seizures.
- Take medications to help manage your mood.
Why are tricyclic antidepressants so toxic in overdose?
TCAs are rapidly absorbed in the gastrointestinal tract. However, following an overdose, owing to the inherent anticholinergic effects, TCAs may decrease the gastrointestinal motility and cause delayed absorption and toxicity. Coingestion of other anticholinergic medications may cause more erratic absorption.
What is the most common local adverse reaction to local anesthetic?
Most emergencies are not due to reactions to the local anesthetic itself, but to the anxiety associated with the injection. The most common reaction is the psychogenic response commonly known as syncope, or fainting. The second most common reaction is hyperventilation or anxiety attack.
What are the early signs of CNS toxicity from injected local anesthetics?
Initial signs and symptoms include agitation, confusion, dizziness, drowsiness, dysphoria, auditory changes, tinnitus, perioral numbness, metallic taste, and dysarthria. Without adequate recognition and treatment, these signs as symptoms can progress to seizures, respiratory arrest, and/or coma.
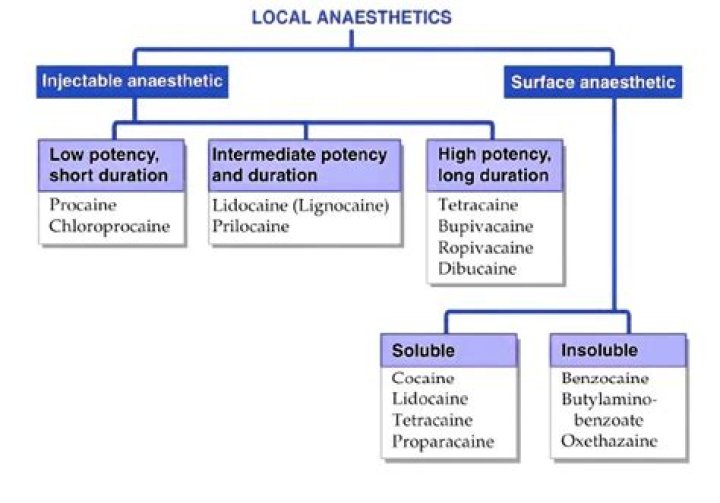
Which of the following is a tricyclic antidepressant?
Drugs in this group include amitriptyline, imipramine, desipramine, doxepin, nortriptyline and others. Desipramine and nortriptyline are used as tricyclic antidepressant as they are less-sedating. TCAs are thought to affect depression by inhibiting synaptic reuptake of norepinephrine and serotonin.
What are atypical antidepressants for postoperative depression?
Atypical antidepressants include venlafaxine and mirtazapine. Both these drugs should be continued throughout the perioperative period. About 70–80% of the patients respond to antidepressant medications, and at least 50% who do not respond to antidepressant do respond favourably to electroconvulsive therapy (ECT).
Can anaesthetics interact with drugs prescribed for psychiatric patients?
Abstract Many patients with psychiatric illnesses are prescribed long-term drug treatment, and the anaesthesiologist must be aware of potential interactions with anaesthetic agents.
Should abrupt withdrawal of tricyclic acid (TCAs) be avoided?
Abrupt withdrawal of TCAs should be avoided because of the risk of mainly cholinergic symptoms. 2 In addition, withdrawing a TCA may precipitate a relapse of the condition for which it is being used.