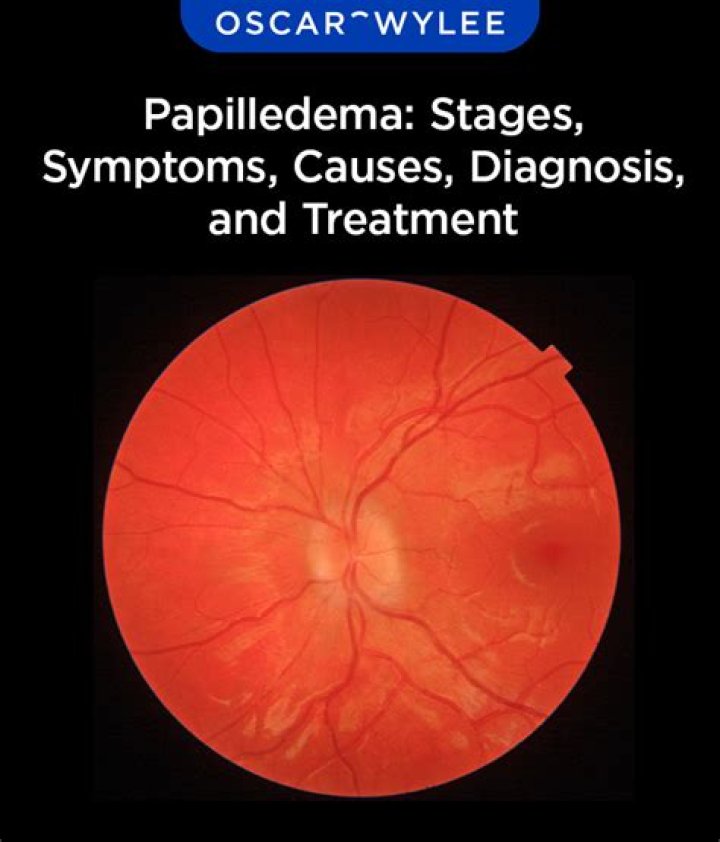
What is the most common cause of papilledema

Michael Henderson
Published Apr 16, 2026
The most common causes of papilledema without IIH were intracranial tumor, intracranial hemorrhage, and cerebral venous sinus thrombosis (Table 1).
What is the cause of papilledema?
Papilledema occurs when increased pressure from the brain and cerebrospinal fluid is placed on the optic nerve. This causes the nerve to swell as it enters the eyeball at the optic disc. There are some serious medical conditions that can cause this increased pressure to develop, including: head trauma.
How common is Papilledema?
Papilledema is not common, but signs and symptoms include headaches, vomiting and nausea, ringing in the ears, blurry or double vision or visual blackouts. Papilledema is a condition in which your optic nerves swell because of high brain pressure.
Can Papilledema be cured?
Papilledema isn’t usually an issue on its own. It can typically be treated by draining extra CSF fluid, which reduces swelling. Symptoms then disappear in a few weeks. Swelling or injury to your brain can be serious and life-threatening.What kind of brain tumor causes Papilledema?
Spinal cord lesions Spinal canal tumor is an unusual cause of high ICP and can result in the development of papilledema. Most of these spinal tumors are intradural, but extradural spinal tumors can also cause high ICP.
Is papilledema rare?
Papilledema or papilloedema is optic disc swelling that is caused by increased intracranial pressure due to any cause. The swelling is usually bilateral and can occur over a period of hours to weeks. Unilateral presentation is extremely rare.
Can hypertension cause papilledema?
). The mechanism behind this phenomenon is poorly understood, but it may be related to a hypertension-related increase in intracranial pressure, and hence is considered true papilledema.
What medications can cause papilledema?
- Corticosteroids.
- Isotretinoin.
- Lithium.
- Tetracycline.
Does papilledema show up on MRI?
Magnetic resonance imaging (MRI) signs associated with papilledema include posterior flattening of the globe, protrusion of the optic nerve, widening of the optic nerve sheath, tortuosity of the optic nerve,16–18 and presence of optic nerve head hyperintensity on diffusion-weighted imaging.
Can stress cause optic neuritis?In fact, continuous stress and elevated cortisol levels negatively impact the eye and brain due to autonomous nervous system (sympathetic) imbalance and vascular dysregulation; hence stress may also be one of the major causes of visual system diseases such as glaucoma and optic neuropathy.
Article first time published onCan you go blind from IIH?
The results of this study suggest that approximately 1-2% of new cases of IIH are likely to become blind in a given year. This contrasts with rates of between 4-10% reported previously in hospital-based studies, but may be a more accurate figure for the population as a whole.
Can high blood pressure cause optic nerve swelling?
A sudden increase in blood pressure can also cause the optic nerve to swell. Along with vision changes, which may include dimmed or double vision, swelling of the optic nerve can cause symptoms such as headaches, nausea, and vomiting.
What causes intracranial pressure?
Increased ICP can result from bleeding in the brain, a tumor, stroke, aneurysm, high blood pressure, or brain infection. Treatment focuses on lowering increased intracranial pressure around the brain.
Is Papilledema always bilateral?
The disc swelling in papilledema is almost always bilateral, although it may be very asymmetric, making it appear unilateral. In papilledema, the elevated CSF pressure disturbs the normal gradient between intraocular pressure and retrolaminar pressure, resulting in increased tissue pressure within the optic nerve.
What are the four stages of increased intracranial pressure?
Intracranial hypertension is classified in four forms based on the etiopathogenesis: parenchymatous intracranial hypertension with an intrinsic cerebral cause, vascular intracranial hypertension, which has its etiology in disorders of the cerebral blood circulation, meningeal intracranial hypertension and idiopathic …
Does glaucoma cause Papilledema?
If glaucoma is a disease that is due in part to decreased intracranial pressure, it then serves as the conceptual opposite to idiopathic intracranial hypertension (IIH). Idiopathic intracranial hypertension is a potentially blinding condition that results in papilledema from increased intracranial pressure.
Can sinusitis cause papilledema?
Conclusions: Sinusitis should always be considered in patients with impaired vision, neuritis nervi optici or unexplained papilledema, especially if occurring in association with an upper respiratory infection.
Does a brain tumor always cause papilledema?
Not all patients with raised intracranial pressure develop papilloedema – this depends on the location and size of the tumour. Also patients who have previously had papilloedema may not develop it in the future. Seizures, sometimes referred to as ‘fits’, are one of the commonest symptoms of a brain tumour.
What is unilateral papilledema?
The term papilloedema refers specifically to optic disc swelling in the presence of raised intracranial pressure. Truly unilateral papilloedema is rare and poses a diagnostic dilemma. An intact optic nerve sheath is apparently necessary for the development of disc oedema in the presence of raised intracranial pressure.
Can Papilloedema be asymptomatic?
The edema is usually bilateral and, when unilateral, suggests a mass lesion behind the affected eye. Early papilledema is asymptomatic. Only with advanced papilledema does transitory obscuration of vision occur.
Can papilledema be reversed?
Most visual defects associated with papilledema are reversible if intracranial pressure is lowered before there is optic nerve damage. In fact, approximately two thirds of patients included in this study did not show evidence of permanent nerve fiber damage at 1 year of follow-up.
Is papilledema the same as glaucoma?
The net result is a negative cupping effect or swelling of the optic disk – a condition called papilledema, with glaucoma like loss of retinal neurons (17, 26, 33, 78).
Can Papilledema be misdiagnosed?
Therefore, children and young adults are particularly vulnerable to misdiagnosis, such as papilledema. Papilledema due to increased intracranial pressure is associated with optic disc hyperemia and a swollen peripapillary retina, which obscures the retinal vessels at the disc margin.
What are the stages of Papilledema?
Papilledema can be graded using the Frisén scale but remains subjective, as follows: Stage 0 is a normal optic disc. Stage 1 papilledema is a C-shaped halo of disc edema with preservation of the temporal disc. Stage 2 papilledema is a circumferential halo of edema on the optic disc.
How is intracranial hypertension diagnosed?
an assessment of your eyes and vision. a CT scan or MRI scan of your brain. a lumbar puncture, where a needle is inserted into your spine to check for high pressure in the fluid that surrounds your brain and spinal cord.
What drugs increased intracranial pressure?
Drugs most commonly associated with intracranial hypertension include vitamin A (at doses >25,000 IU daily) and related compounds (such as isotretinoin and all-trans retinoic acid), tetracycline-class antibiotics, recombinant growth hormone, and lithium.
Can antidepressants cause intracranial hypertension?
Drug-induced intracranial hypertension is well established,[2] but SSRIs leading to papilledema has been very rarely reported. [4,5] Lithium used previously for treating various psychiatric disorders was known to lead to this complication more frequently.
Can a brain tumor cause your eye to swell?
Eye problems can also occur when a brain tumor exerts pressure on the optic nerve or when pressure within the skull causes the back of the eye (optic disc) to swell (a condition known as “papilledema”).
What autoimmune causes optic neuritis?
Optic neuritis is a syndrome of visual loss due to inflammation of the optic nerve. It is usually either idiopathic or associated with multiple sclerosis. Less commonly, it can accompany other systemic inflammatory disorders such as systemic lupus erythematosus, syphilis, or sarcoidosis.
Can MRI show optic neuritis?
A magnetic resonance imaging (MRI) study of the brain and orbits (the eye sockets) with gadolinium contrast may confirm the diagnosis of acute demyelinating optic neuritis.
Does alcohol cause optic neuritis?
Alcohol is no longer considered to cause toxic optic neuropathy, but alcoholism is associated with much higher incidence of nutritional deficiencies, some of which can cause optic neuropathy.