What is the 3rd stage of hemostasis?

Robert Miller
Published Feb 23, 2026
What is the 3rd stage of hemostasis?
Hemostasis has three major steps: 1) vasoconstriction, 2) temporary blockage of a break by a platelet plug, and 3) blood coagulation, or formation of a fibrin clot. These processes seal the hole until tissues are repaired.
What are the 4 steps of hemostasis?
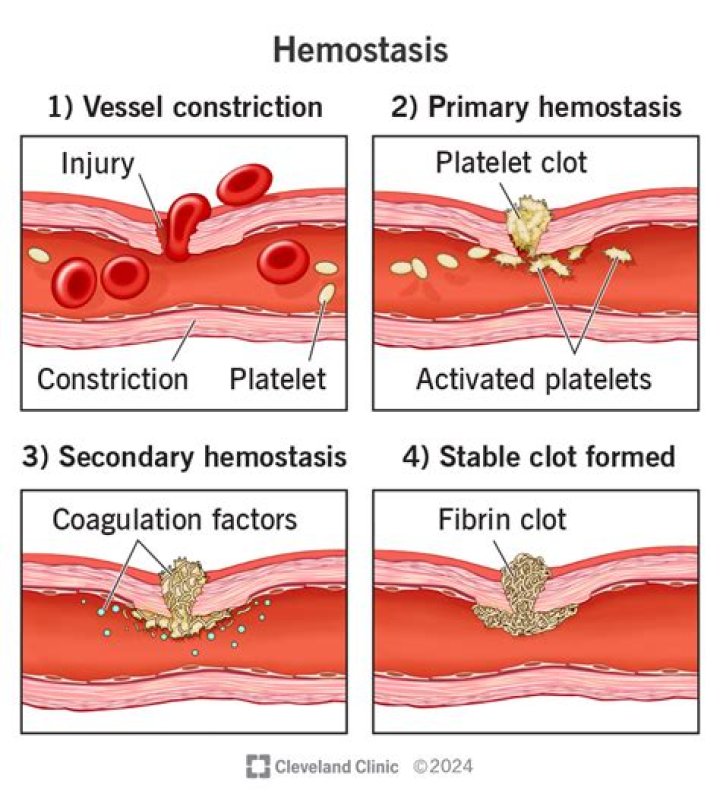
The mechanism of hemostasis can divide into four stages. 1) Constriction of the blood vessel. 2) Formation of a temporary “platelet plug.” 3) Activation of the coagulation cascade. 4) Formation of “fibrin plug” or the final clot.
What happens secondary hemostasis?
Secondary hemostasis refers to the cascade of enzymatic reactions that ultimately results in the conversion of fibrinogen to fibrin monomers. Fibrin monomers are then cross-linked into insoluble strands that serve to stabilize the loose platelet clot formed in primary hemostasis.
What is the coagulation phase?
coagulation, in physiology, the process by which a blood clot is formed. The formation of a clot is often referred to as secondary hemostasis, because it forms the second stage in the process of arresting the loss of blood from a ruptured vessel.
What are the 3 steps to the hemostasis process?
Hemostasis includes three steps that occur in a rapid sequence: (1) vascular spasm, or vasoconstriction, a brief and intense contraction of blood vessels; (2) formation of a platelet plug; and (3) blood clotting or coagulation, which reinforces the platelet plug with fibrin mesh that acts as a glue to hold the clot …
What does a Thrombocyte do?
Thrombocytes are pieces of very large cells in the bone marrow called megakaryocytes. They help form blood clots to slow or stop bleeding and to help wounds heal. Having too many or too few thrombocytes or having platelets that don’t work as they should can cause problems.
Which of the following is the first step of hemostasis?
Hemostasis is the natural process that stops blood loss when an injury occurs.It involves three steps: (1) vascular spasm ( vasoconstriction ); (2) platelet plug formation; and (3) coagulation.
What is the role of extravascular components in hemostasis?
Extravascular cells (fibroblasts and smooth muscle cells [SMCs]) are highly procoagulant and primed to support hemostasis, whereas intravascular (endothelial) cells suppress thrombin generation and fibrin formation.
During which process plasminogen is converted to plasmin?
cleavage
Plasminogen is converted to plasmin by cleavage at the Arg561-Val562 peptide bond by tissue-type or urokinase-type plasminogen activator (tPA and uPA, respectively). Activation of plasminogen by tPA is the major pathway that leads to lysis of fibrin clots. The interaction between tPA and plasminogen is relatively slow.
What does plasmin break down?
Plasmin breaks down fibrin into soluble parts called fibrin degradation products (FDPs). FDPs compete with thrombin, and thus slow down clot formation by preventing the conversion of fibrinogen to fibrin.
What is the vascular phase of hemostasis?
The vascular platelet phase of hemostasis consists of a primary vasoconstriction that serves to decrease blood flow, followed by adherence of platelets to the ruptured endothelium (adhesion) and each other (aggregation).
What role do thrombocytes play in hemostasis?
Thrombocytes (platelets) play an important role in hemostasis, by plugging and repairing damaged blood vessels, thus preventing blood loss. They also participate in a cascade of events that leads to blood clotting by triggering the release of a series of coagulation factors.



