What does the DCT do

Robert Miller
Published Apr 06, 2026
The discrete cosine transform (DCT) helps separate the image into parts (or spectral sub-bands) of differing importance (with respect to the image’s visual quality). The DCT is similar to the discrete Fourier transform: it transforms a signal or image from the spatial domain to the frequency domain (Fig 7.8).
What is the function of DCT?
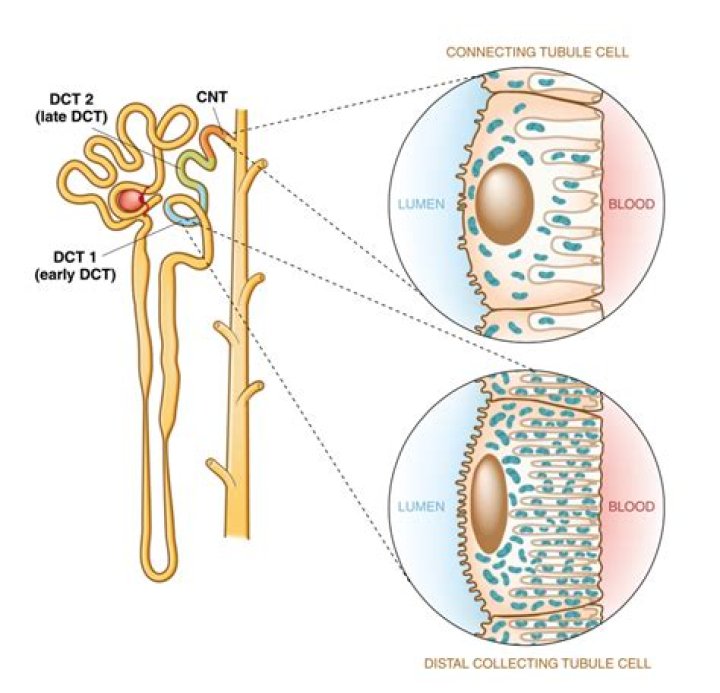
The distal convoluted tubule (DCT) is a short nephron segment, interposed between the macula densa and collecting duct. Even though it is short, it plays a key role in regulating extracellular fluid volume and electrolyte homeostasis.
What happens at DCT?
It regulates pH by absorbing bicarbonate and secreting protons (H+) into the filtrate, or by absorbing protons and secreting bicarbonate into the filtrate. Sodium and potassium levels are controlled by secreting K+ and absorbing Na+.
What is the function of DCT and PCT?
Proximal Convoluted Tubule (PCT) receives primary urine from glomerulus. Distal Convoluted Tubule (DCT) receives urine from the glomerulus. PCT regulates excretion of urine by absorbing excess water from primary urine. In DCT, water and salts are secreted.What is the role of distal convoluted tubule in urine formation?
The distal convoluted tubule (DCT) is responsible for the absorption of HCO3− ions and the secretion of H+ ions, K+ ions and ammonia to maintain the pH of urine and the sodium-potassium balance in the blood.
What do collecting ducts do?
The last part of a long, twisting tube that collects urine from the nephrons (cellular structures in the kidney that filter blood and form urine) and moves it into the renal pelvis and ureters.
What will happen if DCT is removed?
2 Answers. DCT removes any essential ions and salts from the urine before it gets excreted. Thus removal of DCT might lead to loss of these essential elements due to lack of absorption in the body. This might have severe clinical implications and lead to certain deficiencies of mineral ions in the body.
Which is highly coiled PCT or DCT?
The cells present in pct have brush border which is which is capable of absorption. Dct is highly coiled part found in the medula of the kidney.Is PCT highly coiled?
The tubule continues further to form a highly coiled network – proximal convoluted tubule (PCT). A hairpin shaped Henle’s loop is the next part of the tubule which has a descending and an ascending limb.
What happens in loop of Henle?The principal function of the loop of Henle is in the recovery of water and sodium chloride from urine. This function allows production of urine that is far more concentrated than blood, limiting the amount of water needed as intake for survival.
Article first time published onWhat is the purpose of the salt gradient in the kidney?
The kidneys play a critical role in cleaning the blood and controlling the body’s water balance. Unfortunately, their function can be affected by a number of common diseases that can be life-threatening, including infection.
Where is PCT located in kidney?
The proximal tubule is the segment of the nephron in kidneys which begins from the renal pole of the Bowman’s capsule to the beginning of loop of Henle. It can be further classified into the proximal convoluted tubule (PCT) and the proximal straight tubule (PST).
What hormones affect the function of the DCT?
These processes are tightly regulated by hormones, such as parathyroid hormone and 1,25-dihydroxyvitamin D (not shown). Of these transport processes, apical calcium entry through TRPV5 seems to be the rate-limiting step for calcium reabsorption, and the activity of TRPV5 is regulated by several factors.
What is function of DCT for class 10th?
DCT functions for the maintenance of potassium, sodium, calcium, and pH in the blood.
Does the distal convoluted tubule reabsorb water?
The distal convoluted tubule and collecting ducts are then largely responsible for reabsorbing water as required to produce urine at a concentration that maintains body fluid homeostasis.
What happens to walls of DCT when vasopressin is released?
“What happens to the walls of distal convoluted tubule (DCT) of a nephron when vasopressin is released by pituitary into the blood stream ?” … It decreases the loss of water in the urine by increasing the reabsorption of water in the distal convoluted tubule.
What happens to the walls of DCT when vasopressin is released by pituitary?
DCT becomes permeable to water and reabsorb water from the filtrate and make the urine hypertonic.
Which option is common to PCT and DCT?
Similarities Between PCT and DCT Both PCT and DCT occur in the renal cortex. The lumen of both PCT and DCT are lined by the simple cuboidal epithelium. Both PCT and DCT are involved in the reabsorption and secretion. Secondary active transport is involved in reabsorption and secretion in both PCT and DCT.
Where does urine go after the collecting duct?
From the collecting ducts, the urine progresses to the renal pelvis, a widened area of the kidney, and exits through the ureter. The urine passes through the ureters to the urinary bladder.
Are collecting ducts permeable to water?
The basolateral surfaces of the principal cells within the collecting ducts contain aquaporin-based water channels and are always permeable to water. Permeability of the apical surfaces, however, depends upon the presence or absence of ADH.
What hormone acts on the collecting duct?
Aldosterone is a type of steroid hormone that acts primarily in renal collecting ducts to stimulate reabsorption of Na+ as well as secretion of K+ and H+.
What is DCT in kidney?
The distal convoluted tubule (DCT) is the portion of the nephron that is immediately downstream of the macula densa.
Does glucose enter Bowman's capsule?
Any small molecules such as water, glucose, salt (NaCl), amino acids, and urea pass freely into Bowman’s space, but cells, platelets and large proteins do not.
How is water reabsorbed in the PCT?
Reabsorption is when water and solutes within the PCT are transported into the bloodstream. In the PCT this process occurs via bulk transport. The solutes and water move from the PCT to the interstitium and then into peritubular capillaries. The reabsorption in the proximal tubule is isosmotic.
What is the function of PCT Class 10?
The PCT regulates pH of the filtrates by exchanging hydrogen ions in the interstitium for bicarbonate ions in the filtrate. It is also responsible for secreting organic acids such as creatinine and other bases into the filtrate. Proximal convoluted tubule regulate the pH of the filtrate in the kidneys.
What is in renal medulla?
The mature renal medulla, the inner part of the kidney, consists of the medullary collecting ducts, loops of Henle, vasa recta and the interstitium. The unique spatial arrangement of these components is essential for the regulation of urine concentration and other specialized kidney functions.
What is the function of Bowman's capsule?
Bowman’s capsule surrounds the glomerular capillary loops and participates in the filtration of blood from the glomerular capillaries. Bowman’s capsule also has a structural function and creates a urinary space through which filtrate can enter the nephron and pass to the proximal convoluted tubule.
Does loop of Henle have brush border?
The thick descending limbs of the loop of Henle look similar to the proximal tubule, with apical brush borders. The thick ascending limbs are composed of cuboidal cells, but unlike the proximal convoluted tubule, they do not have apical brush borders.
Which hormones regulate the amount of water and salt reabsorbed by the DCT and collecting duct?
The — nervous system causes vasoconstriction of the afferent arterioles, reducing glomerular blood flow and the GFR. Name the hormone that makes the collecting duct more permeable to water so water reenters the tissue fluid and blood rather than being lost in the urine. Which symptoms are seen with diabetes mellitus?
How does the antidiuretic hormone ADH controls kidneys osmosis?
Antidiuretic hormone stimulates water reabsorbtion by stimulating insertion of “water channels” or aquaporins into the membranes of kidney tubules. These channels transport solute-free water through tubular cells and back into blood, leading to a decrease in plasma osmolarity and an increase osmolarity of urine.
What are the importance of ADH and aldosterone in the Osmoregulation process in kidney?
Antidiuretic hormone (ADH) has the primary role in osmoregulation by controlling the amount of urine formation. Body maintain water and electrolytes concentration at a relatively constant level by the mechanism of osmoregulation. Hormone are important signaling molecules that control the regulatory process.



