How do I submit prior authorization to Medicare?

Christopher Anderson
Published Mar 13, 2026
How do I submit prior authorization to Medicare?
To do so, you can print out and complete this Medicare Part D prior authorization form, known as a Coverage Determination Request Form, and mail or fax it to your plan’s office. You should get assistance from your doctor when filling out the form, and be sure to get their required signature on the form.
Can you disclose information to Medicare without consent?
By law, Medicare must have your written permission (an “authorization”) to use or give out your personal medical information for any purpose that isn’t set out in the privacy notice contained in the Medicare & You handbook.
Where do you send a Medicare authorization form?
Once the forms are filled out, you must submit them to Medicare by mail to the following address: Medicare CCO, Written Authorization Dept. PO Box 1270 Lawrence, KS 66044 This address is accurate as of July 2019. Check the end of your form to confirm the appropriate address.
How do I find my Medicare authorization?
To determine if medical authorization is required for a Medicare member, please consult the prior authorization list or call Blue Shield of California Provider Services at (800) 541-6652.
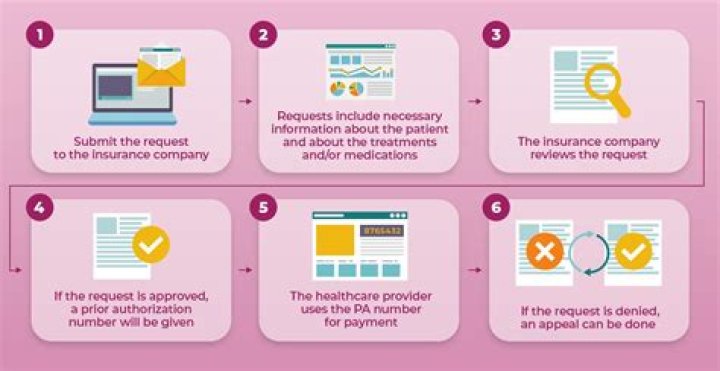
Who requests prior authorization?
Who is responsible for obtaining prior authorization? The healthcare provider is usually responsible for initiating prior authorization by submitting a request form to a patient’s insurance provider.
Which of the following situations may permit disclosure of part 2 information without consent?
There are a few limited exceptions when providers can make disclosures without a patient’s written consent, including: Internal communications. Medical emergencies. Reports of alleged child abuse or neglect (if required by state law)
In which way does the Privacy Rule written authorization differ from the Part 2 consent form?
A: “Consent” is a general term under the Privacy Rule, but “authorization” has much more specific requirements. The Privacy Rule permits, but does not require, a CE to obtain patient “consent” for uses and disclosures of PHI for treatment, payment, and healthcare operations.
What is an authorized representative for Medicare?
An Authorized Representative is a person chosen by a Medicare beneficiary to help with Medicare-related matters, such as the following: Researching and choosing Medicare coverage. Handling Medicare claims and payments. Appealing Medicare coverage decisions.
Can I call Medicare on behalf of someone else?
You can either give verbal permission over the phone for the customer service representative to speak with someone else on your behalf, or fill out an authorization form in advance. Fill out and submit an electronic authorization form online at
Does Medicare require authorization in 2021?
Effective January 1, 2021, prior authorization will be required for certain services on the Medicare Prior Authorization List. This link can also be found on Superior’s Prior Authorization and Superior’s Provider Forms webpages. Prior authorization is subject to covered benefit review and is not a guarantee of payment.
What does prior authorization mean in health insurance?
A decision by your health insurer or plan that a health care service, treatment plan, prescription drug or durable medical equipment is medically necessary. Sometimes called prior authorization, prior approval or precertification.