Does viral meningitis show up lumbar puncture?

Christopher Anderson
Published Mar 13, 2026
Does viral meningitis show up lumbar puncture?
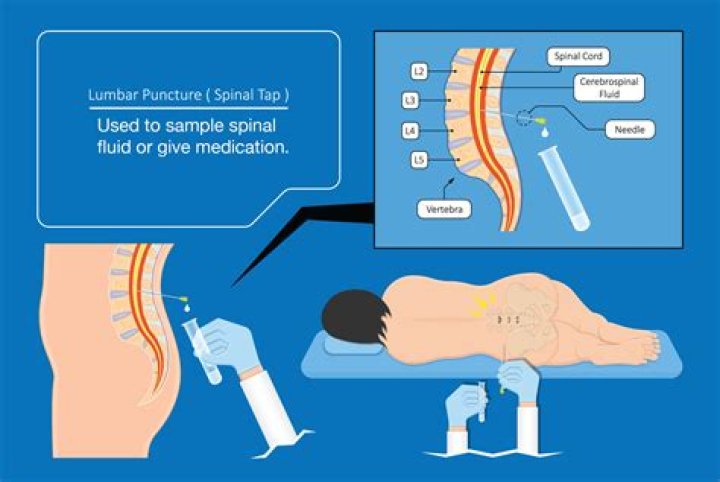
To determine whether a person is suffering from viral or bacterial meningitis, doctors will have to perform a lumbar puncture. This involves collecting a sample of the cerebrospinal fluid (CSF) that surrounds the brain and spinal cord to find out what is causing the meningitis.
What does positive CSF mean?
Your CSF analysis results may indicate that you have an infection, an autoimmune disorder, such as multiple sclerosis, or another disease of the brain or spinal cord. Your provider will likely order more tests to confirm your diagnosis.
When do you need LP for meningitis?
In conclusion, early lumbar puncture rapidly confirms or excludes bacterial meningitis in most cases and should be performed when meningitis is suspected unless there is a specific contraindication (signs of cerebral herniation, signs suggesting a disease other than meningitis or shock).
What does meningitis CSF look like?
Lumbar puncture (LP) cerebrospinal fluid (CSF) findings in bacterial meningitis include the following: Appearance: Clear, cloudy, or purulent. Opening pressure: Elevated (>25 cm H2 O) WBC count: >100 cells/µL (>90% PMN); partially treated cases may have as low as 1 WBC/µL.
Which type of meningitis is worse?
Viral meningitis is the more common and less serious form — it usually clears up on its own in seven to 10 days. Bacterial meningitis is much more dangerous and can be fatal if not treated quickly with antibiotics. Most cases are caused by three different types of bacteria.
Is a lumbar puncture serious?
A lumbar puncture is generally a safe procedure and serious side effects are uncommon. The most common side effects are: headaches, which can last for up to a week – you’ll be given painkillers at the hospital if you need them.
What diseases can be diagnosed with a lumbar puncture?
A lumbar puncture can help diagnose serious infections, such as meningitis; other disorders of the central nervous system, such as Guillain-Barre syndrome and multiple sclerosis; or cancers of the brain or spinal cord.
Why do a spinal tap for meningitis?
So a spinal tap can help doctors find or rule out many diseases or conditions. Most often, doctors order a spinal tap to see if a child has meningitis (infection of the covering of the brain and spinal cord). A spinal tap also can help them look for other conditions that affect the nervous system.
What are the two types of meningitis?
Viral meningitis is the most common type of meningitis, followed by bacterial meningitis. Rarer types of meningitis include chemical and fungal meningitis. The most common types of bacterial meningitis are meningococcal, pneumococcal, TB, group B streptococcal and E.
How do u catch meningitis?
The infection is usually spread by people who carry these viruses or bacteria in their nose or throat, but are not ill themselves. The infection can also be spread by someone with meningitis, although this is less common. It’s possible to get meningitis more than once.
What is the recovery time for a lumbar puncture?
Complications include slight back pain, stiffness in the neck and low grade fever, which should resolve within about a day after the procedure. Recovery from a blood patch is therefore quite quick.
How to diagnose meningitis?
Headache, fever, and stiff neck are the most common symptoms of meningitis. Confusion or lethargy can also be present. Physicians usually make the diagnosis by performing a lumbar puncture ( spinal tap) and evaluating the cerebral spinal fluid (CSF).
What is a normal lumbar puncture result?
In general, though, lumbar puncture results are either normal or abnormal, and if abnormal, there can be an array of causes. Various values measured in a lumbar puncture include the CSF appearance, pressure and total protein, as well as glucose, cell count and the presence of microorganisms or cancer cells.
What is the best treatment for bacterial meningitis?
Commonly used meningitis treatments include a class of antibiotics called cephalosporins, especially Claforan (cefotaxime) and Rocephin (ceftriaxone). Various penicillin-type antibiotics, aminoglycoside drugs such as gentamicin, and others, are also used.