Does hyperventilation cause hypoxemia?

Emma Martin
Published Mar 19, 2026
Does hyperventilation cause hypoxemia?
During recovery after hyperventilation, the transition from hypocapnia to normocapnia is associated with hypoventilation. Be aware that patients may experience significant hypoxemia after hyperventilation.
Can hypoventilation cause hypoxemia?
[21] Hypoventilation does not produce significant hypoxemia in healthy lung, but in the presence of lung diseases, hypoxemia can be severe. One characteristic feature of hypoventilation induced hypoxemia is that it is easily correctible by supplemental oxygen.
How does hypoventilation affect risk for hypoxemia and hypoxia?
Oxygenation is simply the addition of oxygen to the body. You must understand the difference to understand how hypoventilation causes hypoxia. If you hyperventilate with room air, you will lower your arterial carbon dioxide content (PaCO2) significantly, but your oxygen levels won’t change much at all.
What are the 4 causes of hypoxemia?
Common causes of hypoxemia include:
- Anemia.
- ARDS (Acute respiratory distress syndrome)
- Asthma.
- Congenital heart defects in children.
- Congenital heart disease in adults.
- COPD (chronic obstructive pulmonary disease) exacerbation — worsening of symptoms.
- Emphysema.
- Interstitial lung disease.
Are hypoxia and hypoxemia the same?
Hypoxemia (low oxygen in your blood) can cause hypoxia (low oxygen in your tissues) when your blood doesn’t carry enough oxygen to your tissues to meet your body’s needs. The word hypoxia is sometimes used to describe both problems.
What are the five physiological causes of hypoxemia?
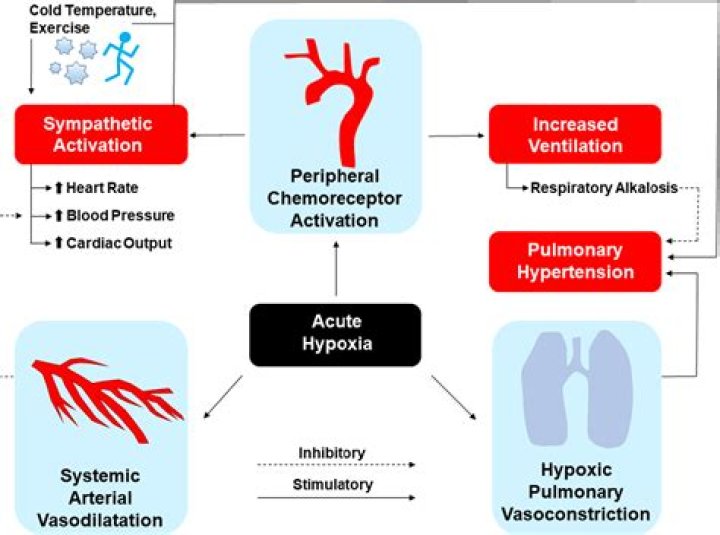
Hypoxemia is caused by five categories of etiologies: hypoventilation, ventilation/perfusion mismatch, right-to-left shunt, diffusion impairment, and low PO2.
How does hypoventilation decrease cause hypoxemia?
Starts here5:26Hypoventilation and Hypoxemia Explained Clearly – RemasteredYouTube
What happens hypoxic hypoxia?
Hypoxic hypoxia (hypoxemic hypoxia): In this type of hypoxia, the tissues do not have enough oxygen because there is a lack of oxygen in the blood flowing to the tissues. Hypoxic hypoxia can be caused by inadequate breathing as well as other causes.
What is the most common cause of hypoxemia?
Some of the most common causes of hypoxemia include: Heart conditions, including heart defects. Lung conditions such as asthma, emphysema, and bronchitis. Locations of high altitudes, where oxygen in the air is lower.
What are symptoms of hypoxia and hypoxemia?
Symptoms
- Changes in the color of your skin, ranging from blue to cherry red.
- Confusion.
- Cough.
- Fast heart rate.
- Rapid breathing.
- Shortness of breath.
- Slow heart rate.
- Sweating.
How is hypoxia and hypoxemia diagnosed?
In general, hypoxia and/or hypoxemia is diagnosed by physical examination and by using oxygen monitors (pulse oximeters), determining, the oxygen level in a blood gas sample and may include pulmonary function tests.
How does hypoventilation cause hypoxemia?
How Does Hypoventilation Cause Hypoxemia? Hypoventilation is a common cause of too little oxygen in the blood. When breathing room air, CO2 takes up space in the alveoli, leaving less room for oxygen. Let’s see how big an effect this is.
Does hyperventilating with room air increase or decrease oxygen levels?
If you hyperventilate with room air, you will lower your arterial carbon dioxide content (PaCO2) significantly, but your oxygen levels won’t change much at all. On the other hand, if you breathe a high concentration of oxygen, but don’t increase or decrease your respiratory rate,…
What is normal PaO2 in a patient with hypoxic ventilation?
Normal PAO2 is about 100 mmHg, so this is quite hypoxic, especially since the alveolar PAO2 is always a little higher than the arterial PaO2. If it weren’t, oxygen would not flow out of the alveoli into the blood — it would stay in the alveoli. That’s a five-fold increase in alveolar oxygen without changing ventilation at all.
How is hypoxemia due to V/Q mismatch corrected?
Hypoxemia due to V/Q mismatch can be easily corrected by supplemental oxygen therapy Widened A-a oxygen gradient is another feature of V/Q mismatch. Some common causes of hypoxemia due to V/Q mismatch include asthma, COPD, bronchiectasis, cystic fibrosis, interstitial lung diseases (ILDs), and pulmonary hypertension.